Sepsis
Understanding Sepsis and Its Management
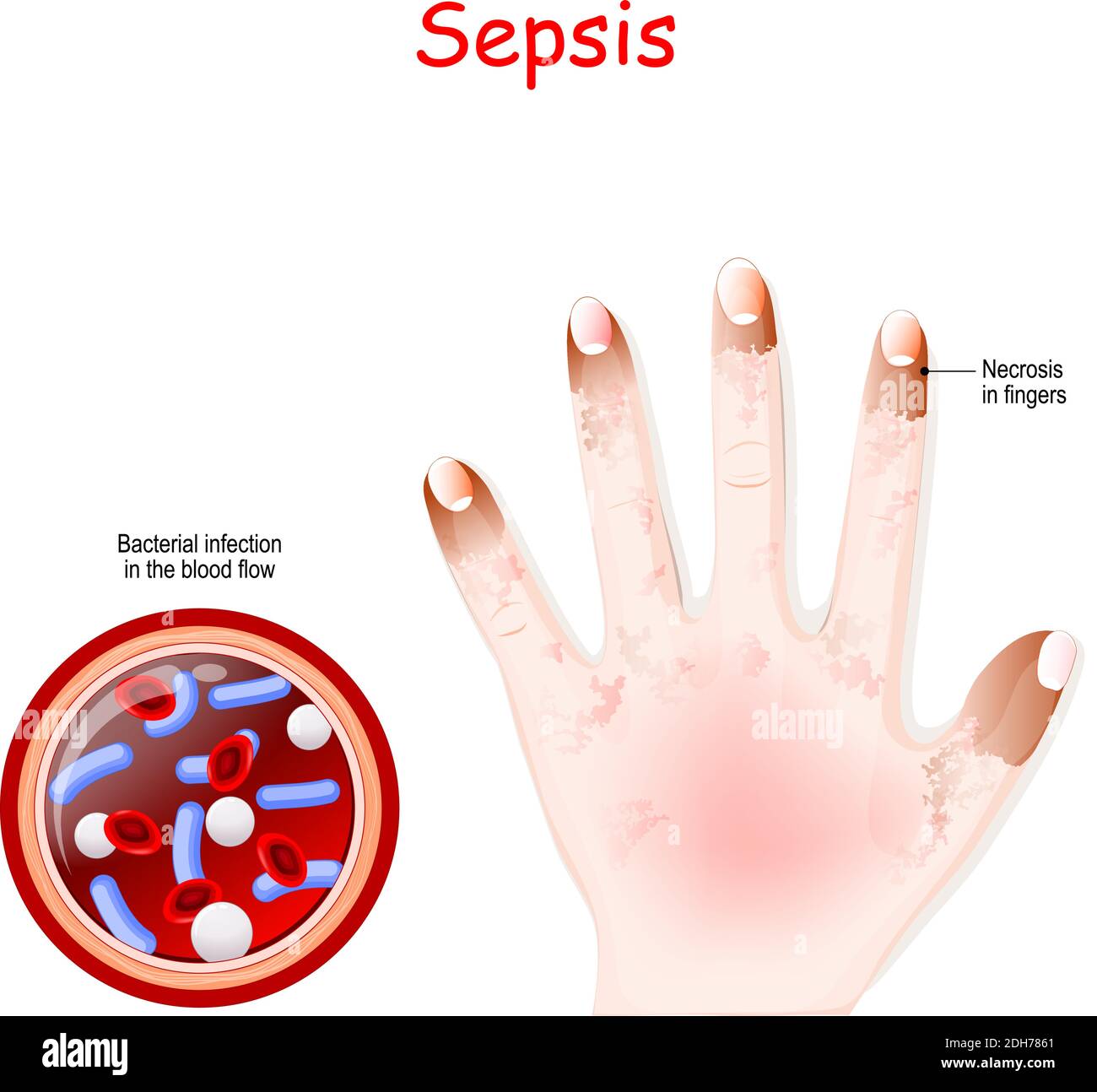
Sepsis is a life-threatening condition that occurs when the body's response to infection triggers widespread inflammation, leading to potential organ damage and failure. Early diagnosis and prompt treatment are critical for improving outcomes.
Causes of Sepsis:
Sepsis can result from bacterial, viral, or fungal infections. Common sources include pneumonia, urinary tract infections, abdominal infections, and bloodstream infections.
Symptoms may include fever, chills, rapid breathing, confusion, low blood pressure, and a weak pulse. Without treatment, sepsis can progress to septic shock, a critical condition requiring intensive care.
Initial Management:
Immediate management of sepsis involves stabilizing the patient, ensuring proper oxygen levels, and initiating intravenous fluids. Early administration of broad-spectrum antibiotics is crucial to control the underlying infection.
Treatment Strategies:
Treatment may involve antibiotics, intravenous fluids, vasopressor medications to maintain blood pressure, and oxygen therapy. In severe cases, mechanical ventilation and dialysis may be required to support organ function.
Close monitoring in an intensive care setting is often necessary to track progress and address complications.
Prevention and Recovery:
Preventing sepsis includes proper vaccination, good hygiene practices, and prompt treatment of infections. Early recognition and intervention are key to improving survival rates and minimizing long-term complications.
In conclusion, sepsis is a medical emergency that requires immediate attention. Awareness of its signs and seeking urgent medical care can significantly reduce the risk of severe outcomes.